T: 01822 851370 E: [email protected]
Visit RSN Survey about life in rural England to find out more.
July Edition of Casebook from the Rural Health and Care Alliance

July 2020 Edition
Welcome to your July edition of Casebook, a dedicated, monthly e-newsletter for Rural Health Care Alliance members. This month, e-enabled approach under threat, local lockdowns, the reality of life in a care home during the pandemic, the challenges of a second wave, homelessness, and its implications. Plus, a feature article from one of our members the Cornwall Partnership NHS Foundation Trust; best Practice from Linkage Sensory Library Bus; and an update from The National Centre for Rural Health and Care on Research, Parliamentary Inquiry, Research, Funding Opportunities and much more. Happy reading!
NEWS COMMENTARY
Huawei decision 'may delay 5G by three years and cost UK £7bn'
Looks like rural areas may face the brunt of our withdrawal from Huawei according to this article. This could have a significant impact on the roll out of e-medicine in rural settings. This story tells us small towns and rural areas across the UK will be hardest hit by delays of up to three years in the rollout of 5G mobile technology. Experts have said after ministers announced that Huawei will be stripped from networks by 2027.
The total cost to the economy could exceed £7bn, according to research analysing the potential cost of eliminating the Chinese equipment supplier in response to US sanctions and pressure from about 60 rebel Tory MPs.
The Huawei dispute is only one part of a wider UK-China struggle.
Oliver Dowden, the culture secretary, announced a U-turn on the role of Huawei in 5G networks on Tuesday, earning criticism from China and praise from the US, who said the company poses a threat to national security.
China’s ambassador to the UK branded the decision “disappointing and wrong”. Liu Xiaoming tweeted: “It has become questionable whether the UK can provide an open, fair and non-discriminatory business environment for companies from other countries.”
Full article:
https://www.theguardian.com/technology/2020/jul/14/huawei-decision-may-delay-5g-rollout-by-three-years-and-cost-uk-7bn-
Ministers can intervene if councils slow to act on local lockdowns, says Johnson
Looks like the pressure is about to ramp up considerably on local authorities as the challenge and blame for local lockdowns is set to be passed to them. This story tells us: Ministers will gain new powers to intervene if local authorities do not act quickly enough against coronavirus outbreaks Boris Johnson has said.
In a series of tweets, Johnson announced ministers would be able to close “whole sectors or types of premises” in a given area, impose localised stay-at-home orders, prevent people entering or leaving certain areas, limit the maximum number of people at a gathering and reduce transport in local areas. This would be “guided by evidence”, he said.
Johnson added the details would be outlined in draft regulations published next week.
From Saturday, local councils have gained greater powers to help avert local lockdowns, including the ability to shut down shops, events and close public outdoor spaces.
Full article:
https://www.theguardian.com/politics/2020/jul/18/ministers-to-gain-powers-to-impose-localised-restrictions-johnson-says
'We were lambs led to slaughter': life inside a care home during Covid-19
This is absolutely shocking witness testimony. It tells us: Those of us who work in health and care have all dealt with death: it’s part of our job and we know it’s going to happen. But the coronavirus crisis has altered the dynamic. Over the past few months, the care home I work in has felt like death’s waiting room. We were told that even critically ill people would not be taken to hospital and we felt helpless as we lost nearly a third of our residents.
At the end of March, we received a man from the local hospital. I was doing my rounds with a nurse when we walked into his room and saw he had all the symptoms of coronavirus. We looked at each other and knew that this was just the start. All night, we shared our anxieties for our residents, our families and ourselves. It was the first time I had felt fear at work.
Within a week, the patient was moved downstairs to a high-security dementia unit because that was felt to be the most appropriate place for him. He had not been tested for Covid-19. Less than a week later, there were many people on the unit with fevers.
Soon, staffing levels began to drop because people were getting seriously ill. At least three members of staff were hospitalised for extended periods of time. There were times when we were at 50% staffing capacity. We still didn’t have adequate personal protective equipment (PPE). Whenever I raised the issue in team meetings, I was snapped at.
We weren’t tested before or after the lock-in. The PPE we had was still not adequate. We had dust masks and gloves with no eyewear. At one point, management sent out a text asking if anybody had any spare bed sheets that could be fashioned into washable gowns.
The lock-in served no purpose. Coronavirus was still present in the care home, and more staff became ill.
The prime minister, Boris Johnson, has since said that care homes were to blame for the UK’s high death toll. To make such a claim after thousands of us put our lives on the line to protect our residents is devastating. We are care workers; our job is hard, but we do it for our residents. But things need to change.
Full article:
https://www.theguardian.com/society/2020/jul/17/lambs-led-slaughter-life-inside-care-home-covid-19
Coronavirus: senior doctors warn second wave could 'devastate' NHS
Scary stuff and I suspect rural areas could be at the forefront of the impacts anticipated here. This story tells us: Senior doctors are pleading with the public to help prevent a second wave of coronavirus that could “devastate” the NHS, amid concern at mixed government messages about face masks and returning to work.
Prof Carrie MacEwen, chair of the Academy of Medical Royal Colleges, said medics and healthcare workers felt “totally reliant on the public understanding that this has certainly not disappeared and could come back and cause even more suffering for the population.”
Dr Alison Pittard, head of the Faculty of Intensive Care Medicine, also warned the NHS could be “overwhelmed” by a second wave coinciding with seasonal flu and the consequences of the backlog of treatment for serious illnesses including cancer.
“People might think Covid is over with, why do I have to wear a face mask,” she said. “But it isn’t over. We still have Covid patients in intensive care. If the public don’t physically distance and don’t wear face coverings, we could very quickly get back to where we were earlier this year.”
Downing Street has said its scientific advice is that new infections are falling at a rate between 1% and 5% a day across the UK. But on Sunday, the Scottish government confirmed a rise in new cases for the fifth consecutive day with 23 people testing positive – the highest daily rate since 21 June.
Meanwhile in Blackburn and Darwen, where health officials last week ordered new restrictions to reduce virus spread, Dominic Harrison, the director of public health, has said the national tracing system was only managing to reach half of those who had been in close contact with a coronavirus patient.
Full article:
https://www.theguardian.com/world/2020/jul/19/coronavirus-senior-doctors-warn-second-wave-could-cripple-nhs
Coronavirus: Duke of Cambridge says it is time to 'crack homelessness'
There are clear links between health and housing and the leadership being shown on this issue by Prince William is to be applauded. This article tells us: During a visit to The Light Project in Peterborough, Cambridgeshire, he said because of the coronavirus pandemic it is the time to "do something properly".
The drop-in-centre has helped to house more than 150 people in four hotels during lockdown.
One of them, Robert Smale, 55, who had been living in a tent for six years, said: "I've got no intention of going back on the streets again."
During lockdown, councils in England have been given £3.2m from the government as part of an emergency scheme called Everyone In, to house them, aimed at stopping the spread of the virus.
While talking to rough sleepers, the prince said: "This pandemic has been truly horrendous for everyone - I'm really hoping that the slivers of positivity and the slivers of goodness that might come out of this is in the homelessness side of things.
"You'll never have a better chance nationally to crack homelessness and do something properly."
MEMBER FEATURE ARTICLE
Cornwall Partnership NHS Foundation Trust
This month we feature an insightful article and video from Cornwall Partnership NHS Foundation Trust about the accelerated launch of Community Assessment and Treatment Units (CATUs) in response to COVID-19
CATUs ensure frail elderly patients receive treatment closer to home. While admitted to a chair or bed, people receive a medical/nursing/therapy assessment. This provides a diagnosis, multi-agency plan, treatment and discharge to home or another setting. Each CATU has x-ray and point of care testing. Admission is for a maximum of 72 hours.
The CATU is GP and nurse-led with medical and therapy cover provided by Cornwall Partnership NHS Foundation Trust. There are named consultants and a frailty hotline, operates from 8am to 10pm, seven days a week. Elder-care consultants from the acute hospital, the complex care and dementia team and palliative care in-reach into the units or are available via clinical advice lines.
Three units were set up by 6 April 2020 as follows:
- Hayman Ward, Camborne Redruth Community Hospital
- Harbour Ward, Bodmin Community Hospital
- Opal Medical 1 at West Cornwall Hospital
A further Practice GP led CATU opened on 18 May 2020 on Heligan Ward, St Austell Community Hospital.
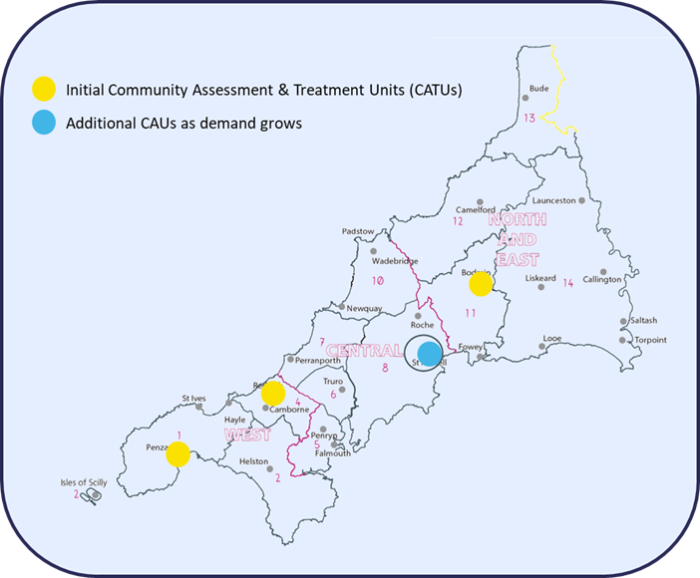
Inclusion criteria:
- Frailty syndrome - falls, dementia, delirium, functional decline, poor mobility, care home resident, Parkinson’s Disease
- Frailty score ≥5 is a guide – older people with frailty syndrome and lower frailty score (2, 3 or 4) considered
- Ceiling of care would be community hospital - completed community treatment escalation plan desirable but not mandatory
- Local older patients with frailty syndromes or low-risk medical problems (NEWS2 <4) who would be for escalation
- Imminent end of life situation that cannot be managed at home and are not for escalation.
Aims:
- Reduce mortality by providing appropriate clinical care for those affected by COVID?19
- Ensuring continuity of essential health and social services
- Protecting clinicians and vulnerable people
- Mitigate some of the disruptive effects of COVID?19 eg shielding, social distancing and movement restrictions, to minimize the negative health impacts.
Objectives:
- Reduce the number of unplanned care episodes in adults with frailty syndrome [meeting CATU criteria] presenting at emergency departments
- Increase the number of frail adult patients managed within the community
- Reduce the number of inpatient days that frail, adult patients [meeting CATU criteria] spend in hospital
- Reduce real [total] cost of providing care to frail adults
- Develop services and skills to support primary care networks to manage care as close to home as possible
Outcomes
Admissions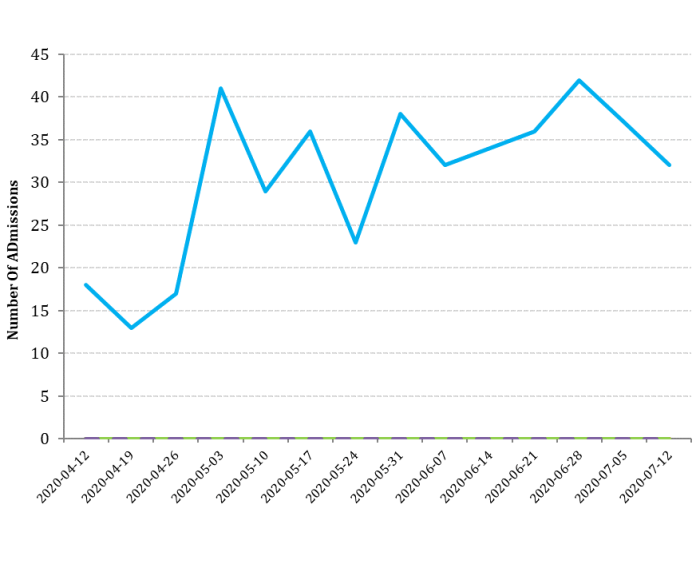
ED frailty attendances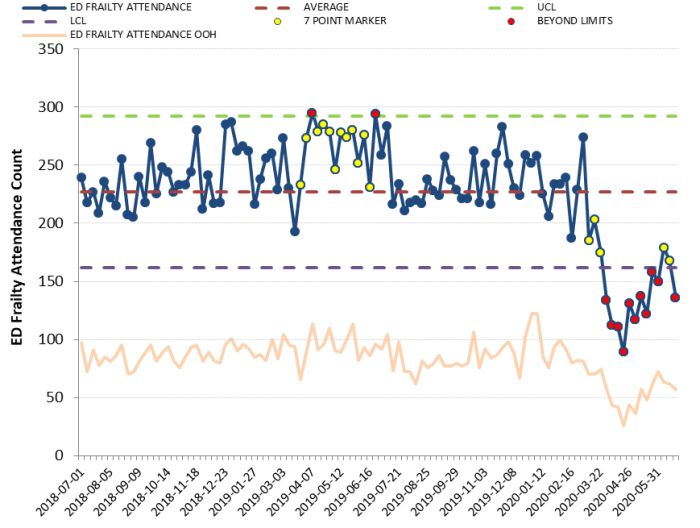
Conclusion
The model has been well received. Regular meetings with staff are developing the long-term workforce model in response to data and demand for the units. This is helping to optimise their use and refine and improve the patient pathway.
Patient feedback has been very positive and comments included: “My stay on Harbour Ward was very good because I got the best treatment and went home to be with my wife.”
Families have also responded positively regarding the end of life wishes, which were made possible.
Video
MEMBER BEST PRACTICE
We are always keen to feature best practice from our members this month we highlight the work of the Linkage Sensory Library and Bus. The Linkage Outreach Project is a unique initiative, funded by the National Lottery Community Fund. The project provides?schools, nursing homes, children’s centres and community groups across Lincolnshire the opportunity to access, enjoy and gain benefit from fully funded sensory resources and facilities. Delivering support to people and places that are difficult to reach, helping to remove the financial and geographical barriers often involved in accessing services in fixed places. The Linkage Sensory Bus is a converted fully- accessible mobile sensory space, packed full of exciting sensory equipment, working with children who have Special Educational Needs and/or Disabilities, and frail older people, (including those with dementia) who are resident in nursing homes.
Why are sensory resources useful?
Sensory occupational therapy is not currently available via the NHS in Lincolnshire, meaning that it can be difficult to access support for sensory difficulties, including Sensory Processing Disorder For children who access sensory therapy and sensory play, there are great benefits- sensory play helps build nerve connections in the brain’s pathways which increases their ability to complete more complex learning. Sensory play also helps with the development of language skills, cognitive growth, motor skills, problem solving skills, scientific thinking, enhancing memory, and supporting social interaction in children. Sensory play is also proven to be calming for children with behavioural issues.
Project Beneficiaries
The bus has enabled Linkage to work with more than 22 organisations a year, many of which are in rural and hard to reach locations. In its first 4 years, the Sensory Bus benefitted over 1,000 children aged 0 to 14 and adults including more than 30 adults aged 80+. Over 95% of those who were beneficiaries of the bus were SEN or had additional needs. Linkage have also taken the Sensory bus on tour to showcase its facilities, including holding sessions for trainee teachers at Bishop Grosseteste University, and attending the launch event of the National Centre for Rural Health and Care.
The Sensory Bus is happy to partner with other organisations and works with Rainbow Stars in Sleaford and has also made contact with the Block Bus in Norfolk, a mobile project offering Lego-based therapy and other interventions. The two projects are learning from each other by sharing ideas, innovative new support methods, and examples of good practice.

Benefits of the Project:
Beneficiary-led support
Children, young people and adults with learning disabilities are integral to the project and shape the equipment, resources and themes used, and are in control of how they choose to use the sensory room on the bus and loans from the library.
The Sensory Library and Bus takes what they call a ‘not one size fits all’ approach, this means that the way the beneficiaries respond to the bus decides the themes of the bus e.g. Under the Sea, Jungle, Outer Space and Garden, which sensory equipment they use, and what they would like to borrow from the Sensory Library. This unique approach to learning has yielded enquiries from as far afield as Scotland, Wales, London, and Portsmouth.
Accessibility
Sensory therapy, play and support are generally found in large towns or cities, and usually at a cost, making it out of the reach of a lot of people, both geographically and economically. By being mobile, the Sensory Bus project provides access to sensory resources out in the community, meaning that beneficiaries do not need to travel outside of Lincolnshire to access support, as instead support comes to them with a particular focus on rural areas.

Affordability
Sensory equipment can be very expensive, and not all resources work for every individual. The project provides multi-sensory equipment to people in their local community and enables them to try it out in their homes at no cost before investing large sums of money in sensory products. Some of the sensory equipment on board the bus is handmade by volunteers and so gives parents/carers ideas of sensory equipment that they can use at home that is not high cost. Sensory boxes are available to purchase from Linkage. Many beneficiaries go on to purchase or make their own equipment.
Promoting ongoing sensory support
The project works with families/carers, school, care centres and community settings so when the 6 weeks of sessions end, they are able to take sensory ideas and approaches and apply them in their own home or setting. The project also plays an important part in signposting beneficiaries to other support services.
The Sensory Bus has also supported trainee teachers from Bishop Grosseteste University to gain further understanding of how sensory equipment can help their future students learn. By providing Continuous Professional Development for trainee teachers, existing teachers, parents, and carers, Linkage is helping to ensure that children and adults across Lincolnshire who have additional needs are getting the best care possible.
Key successes
- The Sensory Library and Bus helps Linkage with early intervention, as the bus supports children of a much younger age group than traditionally worked with through Linkage’s other projects.
- The Lego therapy offered by the Sensory Bus has been happily received by a number of schools as it trains the staff to deliver it while directly working with the children enabling them to continue the work after the sensory bus has left.
- For children, young people and adult beneficiaries, the sensory bus isproviding them with access to a sensory facility and sensory equipment leading them to exercise choice, control and independence; improve their interaction with family members, carers, supporters and be better able to cope in challenging situations. It has improved the beneficiaries’ wellbeing, skills and confidence.
- For families and carers, the sensory bus has improved awareness of sensory resources and opportunities to loan and try out sensory equipment in their homes, this allows parents to try out what works for their children before investing large amounts of money into equipment which may not suit their children, “For parents and carers it makes their job less stressful and provides them with awareness and new ideas around sensory equipment.”
Value for Money
An evaluation of the Social return on Investment provided by the project was carried out by Rose Regeneration. This found that the Sensory Library and Bus to be delivering a social value of £5.35 for every £1.00 invested. Going forward, the only capital costs for the project now will be routine maintenance of the bus. When the large, initial capital outlay is removed from the analysis it is estimated that the project could generate £7.45 for every £1.00 invested in future years.
A short film about the bus:
If your organisation would like to share any case studies or examples of good practice in relation to technology and innovation with other NCRHC members, please email the details to [email protected] . If submitting a case study, these should be between 500 and 1,000 words and include no more than 4 photographs.
NATIONAL CENTRE UPDATE
Research
Last month you’ll recall we said we have a number on research projects in train. Click here to find out more about:
- Recruitment and Retention in Rural Health - University of Birmingham
- Rural Proofing Health Toolkit – Rural England
- Rural Mental Health - Northumbria Healthcare Trust
- Lincolnshire Co-operative Community Pharmacy Project with LIVES
- Recruitment/Retention of Staff in Rural Dispensing Practices, University of Exeter
- Alternative Route into Medicine - Wye Valley NHS Trust/Partners training hub
- Member Research Interests
- Sharing Research Findings
- Research project Example
Parliamentary Inquiry
We have completed two sessions on: coastal issues and on housing. The minutes from both sessions are being checked by witnesses for accuracy and will be available on the National Centre website within the next week or so, check here. The next sessions are on mental health and adult social care on 25 August. If you would like to know more or attend let me know by email.
Rural Health Inequalities Seminar
We have approaching 100 delegates for our seminar on the impact of covid-19 in rural settings on 23 July. It is being chaired by our new eminent board member Professor Sian Griffiths who has significant expertise in the coronavirus having worked on the Hong Kong Government response to SARS. We also have speakers from Nuffield Trust, Airedale NHS Trust, The Campus for Future Living and Support in Mind Scotland. If you couldn’t book, don’t fret, we’ll be emailing you notes after the event.
Rural Proofing Toolkit – Share your Thoughts
This is coming together nicely and we can provide access to key aspects of it for those interested to know more and perhaps help critique where we are so far. To express an interest in getting involved please email.
Campus for Future Living
This is about the development of a tech enabled, community facing health hub with a difference. We are engaging with HEE, the Centre for Ageing Better and the Medical Technology and Innovation Faculty at Nottingham Trent University to plan an exciting new departure in bringing together health and social care through innovation in a remote coastal setting. This initiative has been stimulated by the Towns Funds and could lead to some ground-breaking outcomes for one of the most deprived rural settings in the UK.
Funding Opportunities
This month we focus on four funders namely The Rayne Foundation; Wellcome; Economic and Social Research Council; and the Pixel Fund. To find out more about each of these funds click here
We’d love to hear from you - share what you’re proud of
The RHCA provides news, information, innovation, and best practice. If you have something, you would like us to feature in a future edition, please let us know by clicking here to send us an email.
Spread the Word
If you know of other organisations that you think would benefit from joining the Rural Health & Care Alliance, please click here to email us and let us know.
RURAL SERVICES NETWORK
Up to date news on Health and Care
The Rural Services Network provides a useful source of themed news content and data. Check out the latest news on Health & Wellbeing and Vulnerability, where you’ll find articles on a diverse range of rural issues affecting rural communities . You might also find this research on Over 65 Population Projections and Promoting Cycling for Transport useful too.
| The Rural Health & Care Alliance is a membership organisation administered by the Rural Services Network on behalf of the National Centre for Rural Health & Care. Explore the RHCA service below: |
 |
 |
 |
 |
 |
 |
 |
 |
 |
 |





