T: 01822 851370 E: [email protected]
Dispensing Doctors’ Association

Health and wellbeing boards (HWBs) in England find themselves with an extra six months in which to prepare their local pharmaceutical needs assessment (PNA) – a process that allows local health and wellbeing service coordinators to reconsider the adequacy of their pharmacy network in light of changes to the local demography.
In view of COVID-19, the deadline for producing the 2021 PNA has now been extended to October, with a view to introduction from April 2022.
For dispensing practices – GPs that dispense medicines in rural locations where pharmacies are not viable – PNAs are important documents because they set out in black and white the areas in which a dispensing practice can actually operate (officially known as a ‘controlled locality’) and they acknowledge the services that a dispensing practice offers - albeit that when assessing the need for a new pharmacy that may replace a GP dispensing service, this aspect of the PNA does not carry as much weight in England as it does in Wales.
Since their introduction in England in 2015 (and in Wales in 2022), PNAs have brought some much-needed stability to the pharmacy/dispensing GP network, even though provisions to allow pharmacies that offer ‘unforeseen benefits’ have continued to exert downward pressure on the dispensing GP network in England. In 2019-20, such applications were the most commonly-used in controlled areas where dispensing GPs operate – accounting for eight of the nine pharmacy applications in these areas.
However, as English authorities tussle with their pharmacy network planning, they may benefit from pausing to consider the effect on their planning of online pharmacies. Due to their operation in a virtual rather than terrestrial neighbourhood – and limitations on the services they offer - online pharmacies fall outside the jurisdiction of the PNA and, thus, effectively drive a coach and horses through the PNA planning process.
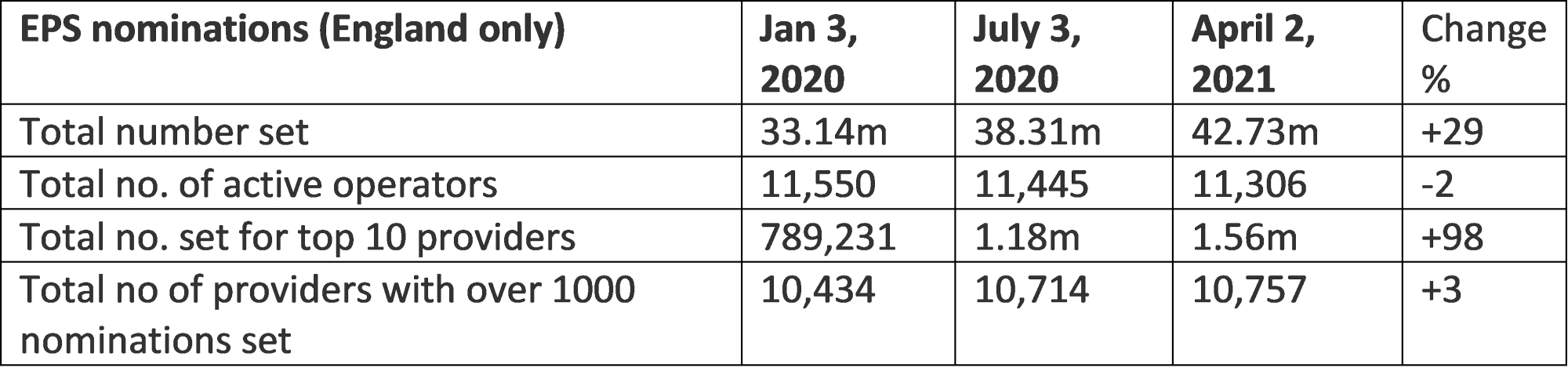
Before COVID, demand for digital prescription services was growing but relatively insignificant. However, lockdown has changed all that: in the period from pre-lockdown to latest figures available at the time of writing (Jan 3, 2020- April 2, 2021) there has been a 30 per cent increase in use of the electronic prescription service in England, a process that allows people to digitally nominate pharmacies, including mail order businesses, to fulfil their prescriptions. Latest figures show that of the top 10 pharmacies nominated to handle EPS scripts, two online only operators alone accounted for just over one million EPS nominations, and collectively grew their business by over 3,800 nominations in just one week.
Online pharmacy Mypharmacy.co.uk has reported that between 2018 to February 2020, the business observed steady year-on-year growth of around 10 per cent. However, during the lockdown period March 2020 - July 2020 online sales increased by 50 per cent, with a 45 per cent increase in customer numbers.
More evidence for the move online is available from The Health Foundation that shows that during the first lockdown, some 45 per cent of UK adults ordered a repeat prescription online and 21 per cent used email/text/app for communicating with a healthcare professional.
A recent paper from consultant Deloitte concludes: “The pandemic is rapidly changing our behaviour toward online channels, and the shifts are likely to stick post-pandemic", citing convenience and greater choice as just two of the reasons consumers will continue to shop online.
Rural roadmap
It’s a moot point whether lockdown healthcare practices will continue throughout, and after, the lockdown recovery period in rural areas where the demographic is older and where digital illiteracy and/or lack of connectivity is more prevalent than in urban areas.
In a recent rural proofing toolkit, Rural England suggests that traditional dispensing GP services such as prescriptions delivered to village shops for remote collection may present a solution to the unique challenges of delivering healthcare services in remote and rural areas, where technology, for whatever, reason cannot fill the gap.
Mohammed Yasir, who runs a traditional bricks and mortar pharmacy in Lancashire alongside the mypharmacy.co.uk online business, agrees that face-to-face pharmacy services have a role moving forward, albeit in a more customer-centric, service-focused way.
Many of the unique services offered by dispensing GP practices – home/remote prescription delivery services, patient’s dispensed medication reviews – are often subsidised by the income provided by the GP dispensing service. For this reason, PNA planners may wish to take note of the unique role these services play in rural communities, when considering the adequacy of their local pharmaceutical network.



