T: 01822 851370 E: [email protected]
Visit RSN Survey about life in rural England to find out more.
Rural, Remote and At Risk - Rural Health
The Nuffield Trust has published a briefing which explores the impact the pandemic has had on the delivery of rural and remote health services in England, highlighting the underlying challenges faced by these services – and outlining how of the challenges faced are different for rural areas in comparison with more urban areas.
Key points in the briefing are:
- Rural and remote areas experienced problems that differentiate them from their more urban counterparts even before the Covid-19 pandemic. However, the pandemic has both exacerbated some of these challenges, as well as thrown up new ones.
- Covid-19 has had a more detrimental effect on hospital waiting times in rural and remote trusts than for trusts in more urban areas. In April 2020, the proportion of patients seen for their first consultant appointment for cancer fell by two-thirds (66%) in rural trusts compared with April 2019, whereas a decrease of 59% was seen in trusts located in more urban areas.
- Activity has fallen particularly dramatically in rural areas. Emergency admissions in April to June 2020 fell by 57% in rural trusts compared with the year before, while they fell by 45% elsewhere. The level of referral for talking therapies – via the Improving Access to Psychological Therapies (IAPT) programme – in rural areas was below half the level in April 2020 than it was a year before.
- The pandemic has exacerbated workforce issues in remote trusts. Remote trusts spend more on temporary staff (8% of their staffing budget) compared with other areas (6%). While the number of hospital and community health staff increased by 7% nationally in the year to June 2020, the workforce of remote trusts grew by only 5% over the same period.
- The underlying financial position of rural and remote services was worse than the position of more urban trusts before the pandemic started, and the pandemic may well have exacerbated this. Remote trusts’ debt was equivalent to more than half (56%) of their annual operating income in 2018/19. Remote trusts also typically do not seem to get their fair share of additional funding that goes into the NHS.
The BBC has reported on the study and you can read their article here.
The Nuffield Trust think-tank says urban areas benefited most from measures put in place to help the NHS cope with the coronavirus pandemic.
Researchers found rural hospitals now faced an uphill challenge when it came to restoring services to normal.
NHS England says that funding reflects the higher costs of delivering care in rural communities.
The Nuffield Trust report says while the number of Covid cases in rural areas was lower than in big urban centres, the pandemic's impact on services has been much greater.
It says the coronavirus crisis highlighted pre-existing problems facing rural trusts.
This graphic below highlights some of the pressures facing rural and remote health care services.
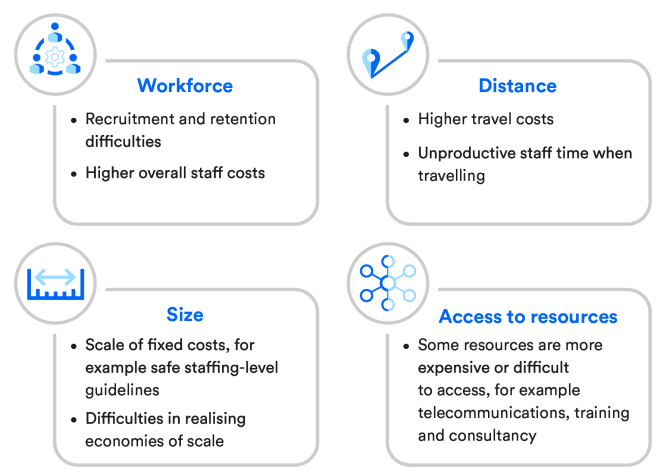 |
In addition, rural trusts often have only a limited capacity to treat any extra patients as they are often already very busy.
Researchers looked at the impact of additional measures put in place in the early days of the pandemic to try and ease the pressure on the health service.
These included the creation of seven Nightingale hospitals in England, a £10bn deal to block book independent sector hospital beds, and extra funding to remodel services to provide hospitals with extra capacity.
The researchers found all these measures were likely to benefit NHS trusts in urban areas more than those serving rural or remote parts of England.
Dr Billy Palmer, senior research fellow at the Nuffield Trust, says there is no doubt the pandemic was a game-changer across the whole health and social care system.
"In the early stages of the pandemic, we saw the NHS put in national measures to help the service to brace itself for a surge in Covid-19 patients.
"Yet our research has found that many of these national policies inadequately considered the needs of rural areas and reflect the long-standing workforce, financial and capacity issues of rural and remote services.
"Rural services are far less likely to benefit from ambitions to use either the urban-centric Nightingale hospitals or the independent sector to clear waiting lists.
"Because of this starting position, rural areas face an ever-growing steep climb to recover from the pandemic without the growing resources, support or capacity available in more urban areas."
One area that researchers focused on was the provision of cancer treatment.
Across the NHS, the number of patients seen by a consultant for a first appointment fell significantly during the early months of the pandemic.
But in rural areas, the fall was 66% compared with 58% in urban areas.
The report says that means that in April of this year, 10,000 fewer patients in rural areas saw a cancer specialist.
The fall in the number of patients admitted for emergency care was also greater in rural areas, at 57% compared with 45% elsewhere.
Prof Richard Parish, chair of the National Centre for Rural Health and Care, said:
"We continue to be concerned that Covid has made a number of rural inequalities worse.
"There doesn't appear to be much short-term prospect of respite. When there is, we still have to make progress towards a level playing field.
"This would involve, for a start, reducing the reliance on agency staff in rural health settings, speeding up rates of hospital discharge and reducing waiting times for elective surgery."
A spokesman for NHS England said the pandemic had presented challenges to the entire health service.
"Funding for health services in more rural parts of the country is already adjusted to reflect the higher costs of delivering care in those communities, including operating hospitals in remote locations and sending ambulances to patients who live there.